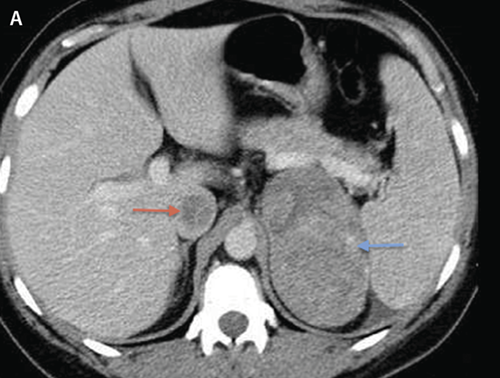
Suprarenal invasion
The incidental detection of kidney cancer has increased due to the dissemination of the use of abdominal imaging methods; such tumors tend to be smaller when compared to symptomatic lesions, according to the observations of Siow et al.. Our study indicated that lesions with isolated hematuria tend to present minor diameters than its counterparts presenting additional symptoms. Such finding may have implications in patients’ prognosis, since other studies still point to the fact that lesion size is one of the most important prognostic factors for RCC.
Our patients had an average overall survival period of 79%, which are in accordance with results showed in previous studies. Evaluating these groups separately, we observe that the association of two or more symptoms to hematuria has repercussions on the global mortality of patients, reducing the survival rate in 40%. Group (3) exhibits a risk 10.5 times greater of death than a patient in group (1).
The higher prevalence of kidney capsule and suprarenal invasion in group (3) correlates with the tendency that lesions presenting with more symptoms tend to be in a more advanced stage.
Patard et al. showed that this finding is more prevalent in a group of patients with systemic symptoms. Similarly, multivariate analysis showed that invasion of the perirenal fatty tissue is strongly associated with specific smaller cancer-specific survival in group (3).
Obviously, the higher prevalence of microvascular invasion and tumoral necrosis established in group (3) revealed to be a relevant finding in our study and it contributed for the worst survival rate in group (3), since microvascular invasion is an independent indicator of a worse prognosis, according to reports from different previous studies. This also occurs in the presence of necrosis.
In our cohort we performed radical nephrectomy for T1 and T2 patients. Despite their smaller size, these tumors had unfavorable location to perform partial nephrectomy. This finding corroborates the fact that when hematuria is present a more aggressive tumor is usually found, even in smaller masses. In this study, the renal function deterioration shown within each group, both due to the increase of serum creatinine and the reduction of clearance only confirms an evolution already indicated in works that emphasize the impact of radical nephrectomy in urological and oncologic surgery on kidney function.
In a previous study, our group reported a recurrence-free survival rate of 82.9% for patients with incidental and 57.3% for symptomatic patients. Schips et al. showed that tendency when comparing asymptomatic patients with symptomatic patients upon the detection of RCC and proved that the presence of symptoms is a parameter of independent impact in the survival of these patients. Lee et al. confirmed this finding in a retrospective analysis of 721 patients submitted to nephrectomy for the treatment of RCC, reiterating that symptomatic presentation is a factor for independent worse prognosis.
The main limitation of this study remains on its retrospective design, with its known disadvantages. Furthermore, patients without hematuria were not evaluated to make a comparative assessment. However, this work highlights the prognostic importance of symptoms in RCC patients.
View article source