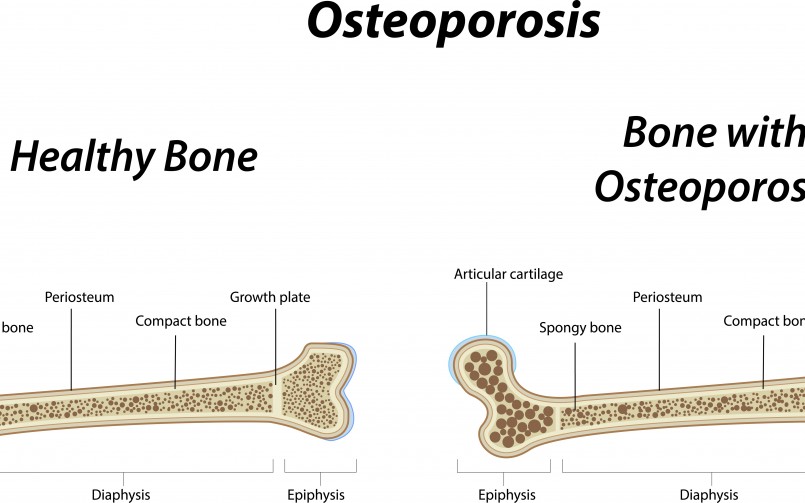
Canadian Health&Care Mall News: Osteoporosis
The worldwide incidence of VCF is 1 in 3 women and 1 in 8 menover 50 years of age. Osteoporosis is the most common condition associated with painful vertebral body compression fractures, resulting in over 500,000 fractures in the United States in 2005.
According to the report of the U.S. Surgeon General, in 2004, osteoporosis-related fractures resulted in more than 432,000 hospital admissions, almost 2.5 million medical office visits, and about 180,000 nursing home admissions. The mean length of stay for management of a VCF was 10.1 days with an average hospital charge of $12,300.
The total United States health care bill associated with lumbar spine fractures in 2007 exceeded 1 billion dollars and it is projected that by 2025, there will be over 3 million osteoporosis-related fractures, with health-related costs of $25.3 billion per year. Our patients treated with kyphoplasty were discharged the same day or the following day. Any reduction in length of hospital stay offers significant healthcare cost savings.
In addition to pain, there are many factors associated with osteoporotic vertebral body compression fractures that threaten quality of life. Compression of the thoracic spine reduces thoracic volume and can inhibit pulmonary function and compression of the abdomen may lead to decreased appetite and bladder incontinence.
Chronic pain and dysfunction can lead to sleep disorders and depression, and decreased activity fosters additional bone loss. Increased mortality has been described following osteoporotic fragility fractures. The mortality rate following a VCF increases 23-34%.
In a review, Mc Girt et al. found level II and III evidence that kyphoplasty resulted in greater improvement of daily activities, physical function and pain relief when compared to optimal medical management for osteoporotic VCF by six months after intervention. Our patients experienced a sustained reduction in pain with a mean pre-operative VAS of 9.0 and a mean postoperative VAS of 2.4; the mean disability index (RMDI) was reduced from a mean of 13.3 pre-operatively to 4.8 following kypho-plasty, and the mean pre-operative EQ5D was 0.308, improved to 0.797 post-operatively.
The reduction in narcotic usage alone would be expected to improve quality of life. Pharma- codynamic changes occur and comorbidities often result in polypharmacy in the elderly; they are at a greater risk for opiod side effects.
A patient with a thoracic compression fracture typically develops kyphosis. The anterior vertebral body compression shifts the center of gravity forward creating a large bending moment. Increased forces on the posterior musculature and ligaments then result in compressive stress.
Adjacent vertebral fractures may follow with further kyphosis and increased pain. As with the treatment of any fracture, four general principles of treatment are applied: reduction of the fracture to restore anatomic alignment, stabilization by fixation, preservation of blood supply, and early and safe mobilization.
Conservative measures such as bed rest, analgesics and bracing do not restore anatomic alignment nor do they improve long term function. Timely repair of these fractures is indicated for effective treatment and to prevent complications associated with inactivity in the elderly.
The consequences of inactivity in this population may be devastating and include de-conditioning with loss of bone, muscle and body mass; orthostatic intolerance with an increased risk of falls; increased risk of deep venous thrombosis, reduced calorie intake; depressed mood and social isolation. Bed rest will lead to continued, if not accelerated bone loss at a rate of up to 2% per week and weight bearing is an important step toward halting or slowing progressive bone loss.
Surgical management may include instrumented fusion, vertebroplasty, or balloon kyphoplasty. Open surgical procedures, including decom-pression and instrumented fusions, are invasive, painful, and require hospitalization, postoperative rehabilitation, and osteopenic bone leads to poor outcomes.
First introduced in the U.S. in 1993, vertebroplasty uses a high-pressure percutaneous injection of polymethyl methacrylate for stabilizing a painful VCF. Balloon kyphoplasty was introduced in 1997 and uses a low pressure injection, thereby reducing the risk of cement leakage. Balloon inflation is intended to restore vertebral height and allow for the low pressure injection.
Both kyphoplasty and vertebroplasty can provide immediate pain relief and allow for an early return to activity. Both procedures allow for bone biopsies for pathological analysis. Additionally, kyphoplasty has been shown to be safe and effective in the correction of non-osteoporotic fractures of the thoracolumbar junction in young patients, with long-term stability.
Potential complications of vertebroplasty and kyphoplasty include extravasation of cement resulting in neural compression, pulmonary embolization, infection, bleeding, and pneu- mothorax. The reported rate of cement extravasation remains lower for kyphoplasty (7-33%) when compared with vertebroplasty (9-47%). Our procedure-related complication rate was 1.6% with cement extravasation occurring in five patients, one of whom required surgical decompression (open re-operation rate of 0.3%).
Additional fractures have been reported following vertebral augmentation procedures but the causal relationship between the procedure and subsequent adjacent vertebral fractures remains unproven as patients with osteoporosis who do not undergo surgery can also develop additional fractures. Following percutaneous procedures, an increased rate of fracture above that of the natural history of the disease has not been demonstrated.
The incidence of fracture following vertebroplasty has been reported to be about 20% within 1 year. This may represent the natural history of subsequent fracture in untreated osteopenic patients. Following an initial fracture, osteoporotic patients not treated with systemic osteoporotic therapy develop an additional fracture at twice the rate (20%) of those on anti-resorptive medication.
Regardless of bone mineral density, age and other clinical risk factors, vertebral fractures confirmed radiographically, even if they are completely asymptomatic, signal impaired bone quality and strongly predict new vertebral and other fractures. The presence of a single vertebral fracture increases the risk of subsequent vertebral fractures 5-fold and the risk of hip and other fractures 2 to 3 fold.
In a matched prospective study, Komp et al. reported a six-month adjacent fracture rate of 37% in patients treated with balloon kyphoplasty and 65% in conservatively treated patients.
In cadaveric studies, Berlemann et al. described a “stress riser” effect weakening a functional spinal unit (2 vertebral bodies and the intervening disc), whereby increased stiffness of the treated vertebra alters the load transfer to the non- cemented adjacent level. Although increased stiffness may theoretically increase the risk of an adjacent fracture by creating a “stress riser”, the kyphotic deformity itself contributes to the compressive effects.
Correction of the kyphosis reduces the compressive forces by reducing the bending moment. Our results demonstrate a lower incidence of adjacent fractures in patients treated with kyphoplasty (4.2%), compared to published rates in untreated patients with osteoporotic fractures (20%). In the current case series, complication rates were low, as were adjacent fracture rates.
This may result from a reduction in bending moment, primarily through restoration of anterior vertebral body height, resulting in the lower incidence of adjacent fractures when compared to published rates in untreated patients with osteoporotic fractures. While we do not provide radiological confirmation of vertebral body height restoration in this series, it has been demonstrated in previous kyphoplasty series.
Another clinically relevant finding is the striking 46% reduction in narcotic usage after kyphoplasty. The typical kyphoplasty candidate is elderly, making narcotic reduction and freedom important for improving mental status, limiting adverse side effects, and reducing polypharmacy in these often complex patients.
There are several limitations to our study. While the VAS was collected prospectively, the RMDI and EQ5D were collected retrospectively, introducing the possibility of recall bias. However, the rate of improvement in RMDI and EQ5D after kyphoplasty follows the same trend as the VAS results, which were collected prospectively. Furthermore, no patient had a worse score post- operatively in any of the three domains, supporting the strength of this trend.
Although some of the data were collected retrospectively, they still capture patients’ perception of pre- operative functioning and assess their satisfaction with the procedure, a key consideration in patient-centered outcomes. Despite the retrospective collection, the data accurately reflect patients’ improvement in quality of life and functional outcome following kyphoplasty.
Multiple VCF aetiologies were included in this group, creating a heterogenous group. However, the results were identical when evaluated as subgroups by aetiology, supporting the efficacy of kyphoplasty across a wide range of pathologies. Additionally, the adjacent fractures captured represent only those leading to symptoms warranting further evaluation. This may have resulted in an underestimate of fractures.
However, this estimate was low (4.1%) and represents the clinically relevant fractures sustained by patients. As this was a cross- sectional study, patient follow up was completed at specific catchment points, March, 2007 and September, 2012, rather than at a standard time period post-procedure and a wide range of follow up was represented (17-1,472 days).
While this may limit reproducibility, it enhances generalizability and demonstrates that the results found in kyphoplasty are rapidly effective and also durable. The follow up range confirms both immediate and sustained pain relief.
Although a well-designed blinded randomized prospective placebo-controlled trial would provide the highest quality of evidence available, it is not necessary nor ethical to further withhold treatment from a patient in severe pain who fails conservative therapy.