Technique for curettage of benign bone tumors
Aggressive benign bone tumors require treatment by curettage of the lesion and packing of the cavity with bone grafts or bone cement. Curettage of the pathologic tissue through a wide cortical window is usually mandatory to avoid the risk of local recurrence. However, large cortical removal for creating the window may weaken the bone and increase the risk of fracture.
Minimally invasive approaches for the treatment of benign bone tumors have been reported in few articles.
Trans-articular arthroscopic excision of benign bone tumors such as chondroblastoma and osteoid osteoma have been reported in the literature. However, trans-articular removal of bone tumors using arthroscopic instruments can cause seeding of the entire joint or spread of tumor cells and potentially may lead to adverse consequences. Moreover, another disadvantage of this technique is the possible cartilage damage during the tumor excision.
Otsuka et al reported a case of a chondroblastoma in the calcaneus with a secondary aneurysmal bone cyst treated by endoscopic curettage. However, this report seems to describe a needle aspiration of an aneurysmal bone cyst rather than a true endoscopic curettage of a chondroblastoma.
Stricker reported three curettage excision of femoral head chondroblastoma using extra-articular endoscopic approach. This technique allowed to avoid hip arthrotomy to make a cortical window in the femoral head. At an average follow-up of 25 months, all three femoral head tumors have healed without recurrence and with no complications related to the approach.
This report presents an innovative minimally invasive technique for curettage and packing of benign bone tumors through a small cortical bone window using the endoscopic instrument. The current study is designed to evaluate the safety and effectiveness of this hypothesis and technique.
METHODS
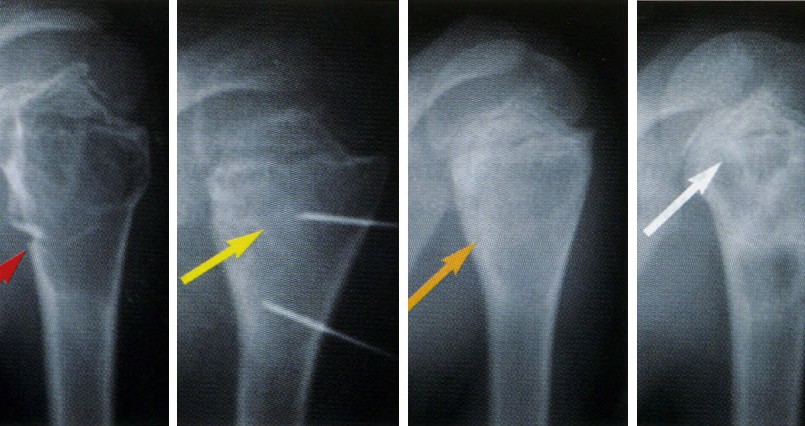
Ten patients with benign bone tumors were treated by curettage of the lesion and packing of the tumor cavity with bone cement or bone allografts using a “minimally invasive endoscopic curettage” (MIEC). We obtained demographic, clinical treatment, and follow-up information from patients’ medical records. The patients had distinctive demographics and tumor distributions. There was a male predilection (6:4), and the patients’ age ranged from 11 to 50 years (mean, 26 years). The anatomical zone distribution of benign bone tumors were as follow: 3 around the knee, 2 in the proximal humerus, 2 in the proximal femur, 2 cases in the distal tibia and 1 case in the distal humerus. The diagnosis included chondroblastoma in 3 cases, aneurysmal bone cyst in 2 cases, fibrous dysplasia in 2 cases and 3 cases with chondroma, giant cell tumor, and non-ossifying fibroma. Plain X-ray in 2 views was performed for all patients pre and post- operatively and on each follow-up visit. Magnetic resonance imaging (MRI) was programmed for all patients preoperatively. In case of juxta-articular lesions a computed tomography, (CT) scan was requested to check the integrity of surrounding cortical bone.
Surgical technique: A pneumatic tourniquet was inflated. The position of the canal was planned preoperatively, and a small skin incision was made accordingly. Using a high-speed burr, a limited orifice of the canal (about 1.5 cm × 2 cm) was made through the cortical bone. Subsequently, under fluoroscopic control, a tunnel was drilled down into the tumor lesion by a finer high-speed burr. The canal was opened and expanded into the tumor cavity. Blinded curettage was performed using a medium curette. Using endoscopic instruments, the precise inspection and curettage of the tumor cavity was planned and performed. Following curettage, under direct view using an arthroscope, the cavity was then burred by high-speed burr and irrigated abundantly. The integrity of the cavity’s walls were checked endoscopically, and the residual cavity was filled with bone cement or bone allograft. Bone cement was used in 4 cases while in 6 other cases the cavities were filled with bone allografts.
In case of chondroblastoma and giant cell tumor, the cavity was soaked with ethanol and phenol as the local adjuvant therapy prior to abundant irrigation. In these cases, the bone cement was used for better detection of possible recurrence.
Post-operative care consisted in immediate active and passive mobilization of the operated limb with early full weight bearing in cases of tumor of the lower extremities. Patients were checked at 2 weeks, and then at 4-month intervals for the 1st year. At each checkup, plain radiographs of the affected area were obtained. The median follow-up was 24 months.
Oncologic results, complication and the functional result were analyzed. Functional results according to the Musculoskeletal Tumor Society (MSTS) functional rating system were evaluated. The functional outcome in these patients was assessed using the functional evaluation system of the American MSTS.